Translate this page into:
Comparison of MRI Findings in Diabetic and Nondiabetic Patients with Rhino-Orbito-Cerebral Mucormycosis
Address for correspondence Prakhar Nigam, MBBS, Department of Radiodiagnosis, M.G.M. Medical College and M.Y. Hospital, CRP Line, Indore 452001, Madhya Pradesh, India (e-mail: prakh3217@gmail.com).
This article was originally published by Thieme Medical and Scientific Publishers Pvt. Ltd. and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Objective
Rhino-orbito-cerebral mucormycosis (ROCM) has emerged as a key concern during the period of coronavirus disease 2019 (COVID-19) pandemic. Diabetes mellitus is a known risk factor for invasive fungal infection. The aim of this article was to study and compare the radiological features of COVID-19-associated ROCM between diabetic and nondiabetic patients using magnetic resonance imaging.
Materials and Methods
A retrospective observational study comprising 78 diabetics and 40 nondiabetics who developed ROCM after COVID-19 was conducted. The imaging data of both groups were analyzed, findings tabulated and compared using statistical methods.
Results
Maxillary and ethmoid sinuses were commonly involved in both groups. Periantral fat and orbits were the most common sites of disease extension. The spread of infection to periantral soft tissue was significantly higher in diabetics (p = 0.049). Diabetics were more likely to have bone, orbit, and brain involvement than nondiabetics, although the difference was not statistically significant. Diabetic patients were the only ones to experience complications such as fungal abscess and cavernous sinus and internal carotid artery involvement. However, a considerable number of nondiabetic patients (22.5%) also had an intracranial extension of disease.
Conclusion
The radiological appearances and common sites of invasion in ROCM are similar in diabetic and nondiabetic patients. The extensive spread of infection to extra-sinus regions can occur in nondiabetic patients with COVID-19 but is less frequent compared with diabetics.
Keywords
COVID-19
diabetes mellitus
magnetic resonance imaging
mucormycosis
Introduction
Rhino-orbito-cerebral mucormycosis (ROCM) is an invasive fungal illness that frequently affects immunocompromised patients. India's mucormycosis epidemiology differs from that of Europe and the United States.1,2,3 In India, uncontrolled diabetes mellitus outweighs other risk factors, such as hematological cancer and organ transplantation, which are significant risk factors in developed nations.1,2,4
Along with the rapid upsurge of coronavirus disease 2019 (COVID-19) cases during the second wave, a substantial rise in the figure of ROCM cases worldwide was seen.5 The high burden of diabetics in India and frequent use of steroids were the major contributors to the development of post-COVID-19 ROCM.6,7,8 Hyperglycemia of diabetes impairs chemotaxis and the phagocytosis process. In addition, the acidosis associated with diabetic ketoacidosis reduces the binding of iron to transferrin, increasing the amount of free iron that encourages fungal growth.9 However, a substantial number of post-COVID-19 patients who were nondiabetic also contracted the invasive fungal infection, possibly due to immunomodulation by severe acute respiratory syndrome coronavirus 2 virus and steroid-induced immunosuppression.10
Rapid progression of ROCM results in cranial nerve palsies and signs of central nervous system involvement within a few hours to days.11 Early magnetic resonance imaging (MRI), because of its excellent multiplanar soft tissue resolution, is useful in determining disease involvement. Extrasinus spread to periantral soft tissue, orbit, or brain often requires a multidisciplinary approach with or without surgical intervention. In light of the high mortality rate, clinicians and radiologists must be aware of the most common locations and routes of infection in all groups. It has been established that diabetes mellitus makes an individual susceptible to fungal infection. However, whether extrasinus spread occurs more extensively in diabetics as compared with nondiabetics has not been evaluated. With this background, we aimed to assess the radiological appearance of ROCM in diabetics and nondiabetics and to compare the findings of both groups with each other.
Materials and Methods
Seventy-eight diabetic and 40 nondiabetic patients diagnosed with ROCM between April 2020 and June 2020 were included in a retrospective observational study at our tertiary care institute. After approval from the institutional ethics and scientific review committee, patients' clinical records and imaging data were accessed and studied. The researchers analyzed medical records of patients who had histological or microbiological evidence of sinonasal mucormycosis, and positive reverse transcriptase-polymerase chain reaction results for COVID-19. Diabetic patients were those who met the standards set out by the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. All patients underwent pathological investigations in the institutional laboratory and imaging using institutional 3T, 97 channel MRI machine.
The MRIs were assessed on the picture archiving and communication system workstation by the authors. The images were initially assessed by two postgraduate resident doctors with more than 2 years of experience as trainees and final reports were prepared after interpretation by the radiologist with 19 years of experience. The radiological characteristics of lesions present in sinonasal and extrasinus areas were noted. The presence of infection in bone, orbit, and brain was determined and disease staging was done on its basis. Stage I disease was defined when lesions were identified within the nasal cavity and the paranasal sinuses, with no extrasinus spread. Stage II patients had orbital involvement. Stage III was suggested by intracranial extension.12,13
Excel spreadsheet was used to compile the data. The data was analyzed using IBM SPSS 26.0. Mean and standard deviation were used to represent normal data. Pearson's chi-squared test was used for the assessment of categorical data. p-Values less than 0.05 were taken as statistically significant.
Results
The mean age of the patients with COVID-19-associated ROCM was 51.56 ± 11 years with a predominance of male patients (68.64%). The duration of onset of symptoms of ROCM after COVID-19 was between 8 and 42 days. Diabetic and nondiabetic patients both had common complaints of facial/periorbital pain or swelling, headaches, and nasal discharge (►Table 1). Maxillary and ethmoids were the most commonly involved sinuses (►Table 1). Bilateral involvement of sinuses was more common than unilateral, with predominance to the right side. There were low signals on T1-weighted images, intermediate/low signals on T2-weighted images, and nonenhancing areas on contrast-enhanced images in the majority of the affected sinuses.
| Characteristics | Diabetic | Nondiabetic |
|---|---|---|
| Mean age (SD) | 54.17 (11) | 46.48 (11) |
| M:F | 55:23 | 26:14 |
| Clinical presentation | ||
| Facial/periorbital swelling | 52 (66.67%) | 22 (55%) |
| Facial/periorbital pain/reduced sensation | 51 (65.38%) | 24 (60%) |
| Nasal blockage | 44 (56.41%) | 17 (42.50%) |
| Headache | 44 (56.41%) | 24 (60%) |
| Fever | 27 (34.61%) | 10 (25%) |
| Nasal discharge | 16 (20.51%) | 5 (12.50%) |
| Ophthalmoplegia | 9 (11.53%) | 8 (20%) |
| Toothache/loosening of tooth | 4 (5.13%) | 0 (0%) |
| Altered sensorium | 3 (3.85%) | 0 (0%) |
| Sinus involved | ||
| Maxillary | 76 (97.44%) | 40 (100%) |
| Ethmoid | 77 (98.72%) | 37 (92.5%) |
| Sphenoid | 61 (78.20%) | 25 (62.5%) |
| Frontal | 49 (62.82%) | 20 (50%) |
| Extrasinus spread to periantral soft tissue | ||
| Periantral fat | 68 (87.18%) | 27 (67.5%) |
| Masticator space | 47 (60.26%) | 13 (32.5%) |
| Infratemporal fossa | 45 (57.69%) | 10 (25%) |
| Pterygopalatine fossa | 27 (34.61%) | 8 (20%) |
| Bone involvement | 37 (47.43%) | 16 (40%) |
| Orbital involvement | ||
| Extraconal fat | 54 (69.23%) | 22 (55%) |
| Intraconal | 42 (53.84%) | 16 (40%) |
| Orbital apex | 11 (14.10%) | 11 (27.5%) |
| Intracranial extension | ||
| Meningitis | 14 (17.95%) | 3 (7.5%) |
| Cerebral edema/cerebritis | 12 (15.38%) | 2 (5%) |
| Intracerebral abscess | 7 (8.97%) | 0 (0.00%) |
| Cerebral infarcts | 21 (26.92%) | 7 (17.5%) |
| Cavernous sinus thrombosis | 3 (3.84%) | 0 (0.00%) |
| ICA thrombosis | 2 (2.56%) | 0 (0.00%) |
Abbreviations: ICA, internal carotid artery; SD, standard deviation.
Periantral fat and orbits were the most common sites of extrasinus spread in both groups (►Table 1). Extension of disease in periantral fat was seen in the form of stranding, better visualized on fat-saturated images, or as an enhancement on contrast administration. Soft tissue lesions with variable postcontrast enhancement or bulky muscles with a heterogenous enhancement suggested the involvement of masticator space. Soft tissue lesion in pterygopalatine fossa with or without expansion suggested its involvement. In all cases with orbital extension, extraconal fat stranding was seen with variable involvement of intraconal fat, extraocular muscles, and orbital apex (►Figs. 1 and 2).

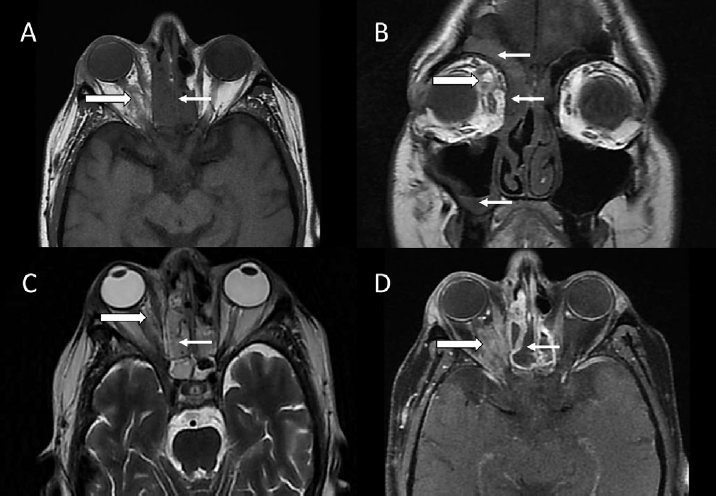
- Coronal T1-weighted (A) and axial T2-weighted fat-saturated (B and C) images of a 40-year-old nondiabetic male showing T1 hypointense and T2 hyperintense soft tissue in the left maxillary sinus (white stars), extending into left extraconal fat through inferior orbital wall (straight black arrow). Similar lesion is seen in the right maxillary sinus in inferior aspect (straight white arrow). Note left premaxillary fat stranding (curved down arrow) and involvement of left nasolacrimal duct (curved right arrow). Axial T1-weighted image (D) at the level of orbits shows normal intraconal fat and extraocular muscles.
- Axial T1-weighted (A), coronal T1-weighted (B), axial T2-weighted (C) and axial T1-weighted fat-saturated postcontrast (D) images of a 60-year-old diabetic female showing soft tissue in bilateral ethmoid sinuses, right frontal, and right maxillary sinuses (small arrows) with areas of nonenhancement on contrast administration. Extension of lesion seen in right orbit (large arrows) with intraorbital fat stranding and heterogenous postcontrast enhancement.
Diabetics have significantly greater extension into periantral soft tissue than nondiabetics (p 0.049). Although diabetics had greater rates of bone involvement, orbital and intracranial extension than nondiabetics, the differences were not statistically significant (p 0.442, p 0.126, and p 0.081, respectively). The vast majority of diabetics were in stage II/III, whereas nondiabetics had lower stages (►Table 2).
| Radiological stage | Diabetics | Nondiabetics | p-Value |
|---|---|---|---|
| Stage I (sinonasal disease) | 20 | 16 | 0.146 |
| Stage II (orbital extension) | 28 | 15 | |
| Stage III (intracranial extension) | 30 | 9 | |
| Total | 78 | 40 |
Discussion
The Mucorales order is responsible for the development of RCOM. Among the fungi that comprise this category are Mucor, Rhizopus, Absidia, Cunninghamella genus, and Apophysomyces elegans.14 Inhalation of spores of these fungi followed by germination in sinonasal mucosa is the common mode of infection. Once inoculated, the spread of infection occurs to surrounding soft tissue, orbit, or brain through direct extension, angioinvasion, or perineural routes.13 Mucorales have the tendency to invade the endothelium of arteries, resulting in thrombosis, ischemia, and gangrene.15
In our study, a subset of patients from both groups had premaxillary/retroantral fat stranding without any obvious erosion of the bony wall of the maxillary sinus. Involvement of periantral fat without bony erosion suggests perivascular/perineural spread.13,16,17 It was found in 74% of the patients evaluated by Yadav et al that periantral soft tissue extension is an initial imaging sign of penetration into fat outside the maxillary sinus related to bone degradation or spread via the perivascular pathway.12 The involvement of periantral soft tissue in our study was more significant in diabetics than nondiabetics. The persistent rise in blood glucose levels, hyperglycemia-induced receptors on vessel walls, and impaired immunity in diabetics facilitate vascular invasion of fungi.
The orbital involvement was common in both diabetics (69.23%) and nondiabetics (55%). Though the ocular extension was higher in diabetics, it was not significant. Diabetics were expected to have a higher degree of ocular involvement due to the presence of factors favoring angioinvasion. However, the invasion through lamina papyracea or nasolacrimal duct was also seen frequently that explains the spread in nondiabetics.
Intracranial spread of the infection was more common in diabetics than nondiabetics, although not significant. Intracranial spread can occur through cribriform plate, along cranial nerves and branches of intracranial vessels.13,18,19 Severe complications of intracranial spread such as thrombosis of cavernous sinus or carotid artery, and severe form of brain involvement in the form of abscess formation were exclusive to diabetics in the present study (►Fig. 3). The impaired chemotaxis and phagocytosis and depressed local inflammatory response could be responsible for fungal complications in diabetics.20

- Axial T1-weighted (A) and T2-weighted (B) images of a 72-year-old diabetic female showing a large irregularly marginated T1 isointense and T2 hypointense lesion in left frontal lobe (large arrows) with central hyperintense area and perilesional edema (small arrows). The lesion causes midline shift with mass effect on adjacent horn of left lateral ventricle. It also shows blooming along its periphery (white curved arrow) on susceptibility-weighted imaging (C) suggestive of fungal elements.
On stratifying the patients on the basis of disease stage, we found that extrasinus involvement was more common in diabetics. However, a substantial number of patients belonging to the nondiabetic group also showed extrasinus spread. There could be several explanations for this. All patients in our study, whether diabetic or nondiabetic, had a history of COVID-19. COVID-19 is associated with altered innate and adaptive immunity due to the release of various inflammatory mediators and virus–host cell interactions, which promote fungal invasion.21 COVID-19 is also a hyperferritinemic condition, where high serum ferritin levels produce excessive intracellular iron deposition, which causes reactive oxygen species, resulting in injury to tissues.22 Tissue injury causes the release of free iron into the bloodstream, which aids in the growth and spread of fungi in the body.23 COVID-19 treatment includes administration of steroids that are hyperglycemic and immunosuppressive agents. COVID-19 patients also suffer from acid–base imbalance.24 Endothelium receptor glucose-regulated protein78 is induced in acidemia and hyperglycemic conditions, allowing Mucorales penetration through the endothelial barrier.25
Our study data suggests disease involvement of orbit and brain in post-COVID-19 nondiabetic patients. However, the extrasinus spread of mucormycosis to periantral soft tissue is more common in diabetics in comparison to nondiabetics. Our study is novel in comparing the two groups radiologically. However, there are certain limitations to our study. First, due to the unavailability of data, we could not correlate the disease severity with the daily blood glucose levels at the time of illness. Second, due to the retrospective character of our investigation and the availability of a single MRI scan per patient, it was not possible to analyze the radiological progression of the disease since its beginning, which would have offered a better understanding of the pattern of disease spread. There is a scope of future multicentric study with a larger sample size for a better understanding of the differential findings between the two groups.
Conclusion
The intracranial spread of mucormycosis can occur in both diabetics and nondiabetics. However, severe intracranial complications were exclusive to diabetic patients. Our study suggested frequent periantral soft tissue invasion in diabetics as compared with nondiabetics. Future analysis through larger multicentric studies may provide us a superior corroborative statement for clinical application.
Author Contributions
A.A. contributed to conceptualization, supervision, project administration, methodology, data interpretation, review, and editing. N.K. was involved in supervision, project administration, methodology, review, and editing. G.M. contributed to draft preparation, methodology, data collection, and validation. P.N. was involved in preparation, data collection, analysis, and interpretation. S.A. was involved in data curation, analysis, and editing. All authors read and approved the final manuscript.
Ethical Approval
The study was approved by the ethics and scientific review committee of M.G.M. Medical College, Indore, Madhya Pradesh, India (approval number: IRB-22/01).
Conflict of Interest
None declared.
References
- European Confederation of Medical Mycology Working Group on Zygomycosis. Zygomycosis in Europe: analysis of 230 cases accrued by the registry of the European Confederation of Medical Mycology (ECMM) Working Group on Zygomycosis between 2005 and 2007. Clin Microbiol Infect. 2011;17(12):1859-1867.
- [CrossRef] [PubMed] [Google Scholar]
- Prevalence, clinical and economic burden of mucormycosis-related hospitalizations in the United States: a retrospective study. BMC Infect Dis. 2016;16(01):730.
- [CrossRef] [PubMed] [Google Scholar]
- Changing epidemiology of an emerging infection: zygomycosis. Clin Microbiol Infect. 2009;15(Suppl 5):10-14.
- [CrossRef] [PubMed] [Google Scholar]
- Mucormycosis in India: unique features. Mycoses. 2014;57(Suppl 3):85-90.
- [CrossRef] [PubMed] [Google Scholar]
- Global and regional diabetes prevalence estimates for 2019 and projections for 2030 and 2045: Results from the International Diabetes Federation Diabetes Atlas, 9th edition. Diabetes Res Clin Pract. 2019;157:107843.
- [CrossRef] [PubMed] [Google Scholar]
- Coronavirus disease (covid-19) associated mucormycosis (CAM): case report and systematic review of literature. Mycopathologia. 2021;186(02):289-298.
- [CrossRef] [PubMed] [Google Scholar]
- Glucocorticoids and invasive fungal infections. Lancet. 2003;362(9398):1828-1838.
- [CrossRef] [PubMed] [Google Scholar]
- A mechanism of susceptibility to mucormycosis in diabetic ketoacidosis: transferrin and iron availability. Diabetes. 1982;31(12):1109-1114.
- [CrossRef] [PubMed] [Google Scholar]
- Immunomodulation in COVID-19. Lancet Respir Med. 2020;8(06):544-546.
- [CrossRef] [PubMed] [Google Scholar]
- Epidemiology and clinical manifestations of mucormycosis. Clin Infect Dis. 2012;54(Suppl 1):S23-S34.
- [CrossRef] [PubMed] [Google Scholar]
- Magnetic resonance imaging in coronavirus disease - 2019 associated rhino-orbital-cerebral mucormycosis (CA-ROCM) - imaging analysis of 50 consecutive patients. Curr Probl Diagn Radiol. 2022;51(01):112-120.
- [CrossRef] [PubMed] [Google Scholar]
- Imaging features of rhinocerebral mucormycosis: a study of 43 patients. Egypt J Radiol Nucl Med. 2018;49(02):447-452.
- [CrossRef] [Google Scholar]
- Rhinocerebrocutaneous mucormycosis caused by Mucor species: a rare causation. Indian Dermatol Online J. 2015;6(03):189-192.
- [CrossRef] [PubMed] [Google Scholar]
- Rhinocerebral mucormycosis caused by Apophysomyces elegans. Am J Rhinol. 1998;12(04):289-292.
- [CrossRef] [PubMed] [Google Scholar]
- Spectrum of MR imaging findings of sinonasal mucormycosis in post COVID-19 patients. Br J Radiol. 2021;94(1127):20210648.
- [CrossRef] [PubMed] [Google Scholar]
- Imaging findings using a combined MRI/CT protocol to identify the “entire iceberg” in post-COVID-19 mucormycosis presenting clinically as only “the tip”. Clin Radiol. 2021;76(10):784.e27-784.e33.
- [CrossRef] [PubMed] [Google Scholar]
- Magnetic resonance imaging in fungal infections of the brain. Top Magn Reson Imaging. 2014;23(03):199-212.
- [CrossRef] [PubMed] [Google Scholar]
- Invasive sino-orbital fungal infections in immunocompetent patients: a clinico-pathological study. Eye (Lond). 2019;33(06):988-994.
- [CrossRef] [PubMed] [Google Scholar]
- Rhinocerebral Mucormycosis. [Updated 2021 Nov 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. Accessed September 21, 2022 at: https://www.ncbi.nlm.nih.gov/books/NBK559288/
- [Google Scholar]
- Hallmarks of immune response in COVID-19: exploring dysregulation and exhaustion. Semin Immunol. 2021;55:101508.
- [CrossRef] [PubMed] [Google Scholar]
- COVID-19 as part of the hyperferritinemic syndromes: the role of iron depletion therapy. Immunol Res. 2020;68(04):213-224.
- [CrossRef] [PubMed] [Google Scholar]
- Pathogenesis of mucormycosis. Clin Infect Dis. 2012;54(Suppl 1):S16-S22.
- [CrossRef] [PubMed] [Google Scholar]
- When uncontrolled diabetes mellitus and severe COVID-19 converge: the perfect storm for Mucormycosis. J Fungi (Basel). 2021;7(04):298.
- [CrossRef] [PubMed] [Google Scholar]





